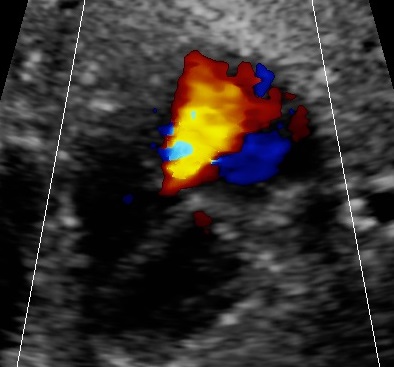
Fetal hyperthyreoidism is the fetal hypersecretion of thyroid hormones. Fetal thyreotoxicosis is the clinical syndrome of hypermetabolism and hyperactivity once the fetus has been exposed to excessive thyroid hormones.1
Fetal hyperthyreoidism is in most cases transient and secondary to maternal Grave’s disease. Other, more rare causes can be mutations of the TSH-Receptor or the McCune-Albright syndrome.2 Grave’s disease is the most common cause of hyperthyroidism in women of reproductive age.3 The prevalence in pregnant women is around 0.1-0.4% and 1-5% of the neonates born to mothers with Grave’s disease develop thyreotoxicosis. Thus the expected incidence of Grave’s disease of the newborn can be estimated to be around 1:25.000 and 1:50.000. Contrary to Grave’s disease of the adult, newborn boys and girls can be equally often afflicted.2
Pathophysiology
IgG antibodies, iodine, thyroxine (T4) and all thyreostatic drugs cross the placenta.1
The fetal thyroid is formed in the 5-6th week of pregnancy and the thyroxine secretion begins in the 10th week. The embryonic needs in earlier stages are fulfilled through the maternal thyroxine. Only after the 18-20th week are the TSH-receptors functional.4,5
The cause of fetal Grave’s disease are the maternal TSHR-Ab of the stimulating type that belong to the IgG class and thus cross the placenta.2 This means that fetal Grave’s disease is typically seen after 20 weeks of pregnancy.1
Clinical Presentation
- fetal sinus-tachycardia (around 180-200 bpm)
- holosystolic tricuspid insufficiency
- IUGR
- Goiter
- Oligo- or Polyhydramnios
- Accelerated bone maturation
- craniosynostosis
- microcephaly
- hydrops fetalis
- premature delivery
- intrauterine fetal demise2,4,6,7
Diagnosis
- patient history
- biochemical examination (fT4, TSH, TSHR-Ab)
- targeted ultrasound examination
Patients with Grave’s disease should always have a measurement of the TSHR-Ab in the beginning of pregnancy, even after ablative therapy.1 Values above 3x the upper limit are associated with fetal and neonatal hyperthyroidism.4 In case the levels of TSHR-Ab increase during pregnancy or if the mother recieves thyreostatic medication a second test should be performed between 18-22 weeks of pregnancy. If these persist, a third test is indicated between 30-34 weeks. Women who recieve anti-thyroid drugs (ATDs) need a measurement of fT4 and TSH every 4 weeks. Ideally thyroxine should be in the upper normal limit or slightly above it, meaning that the least possible dosis of ATDs is used.1
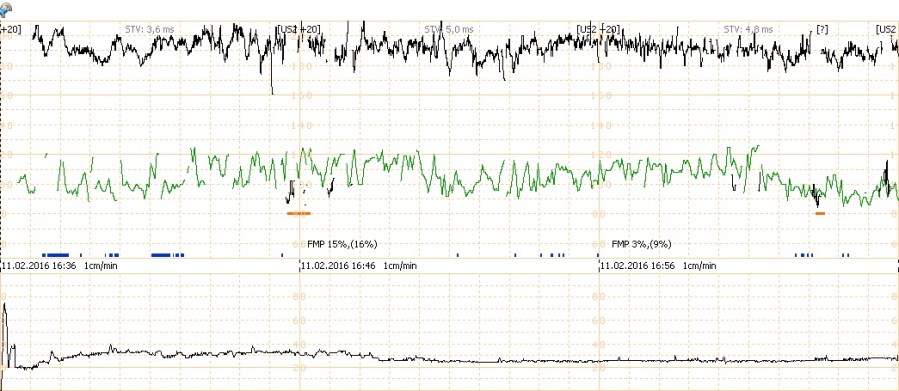
Figure. Cardiotocogram of a patient with fetal grave’s disease in the 31st week of pregnancy.
Indications for targeted fetal ultrasound examination are:
- non-treated maternal hyperthyroidism in the second half of pregnancy, or
- TSHR-Ab above 3x the upper normal limit.1
The monitoring should be every 4-6 weeks after the 20th week of pregnancy. We suggest the documentation of the following:
- fetal heart frequency
- estimate of the amniotic fluid volume
- fetal growth
- Head circumference and possible craniosynostosis
- Thyroid circumference and in case of goiter the vascularisation of the thyroid
- fetal bone maturation (distal femural epiphysis)
- signs of heart-insufficiency, like tricuspid valve insufficiency or ascites.1,2,6,8,9,10
Admittedly there is no optimal monitoring in cases of suspected fetal grave’s disease. Even if the fetal heart frequency returns to normal or if goiter resolves, this does not necessarily mean that the fetus thyroid hormone levels have returned to normal.11 The gold-standard for the confirmation of the diagnosis remains the cordocentesis (percutaneous umbilical blood sampling).5
Fetal hyperthyroidism can be treated with thyreostatic drugs applied to the mother.5 Fetal Grave’s disease typically presents after the 20th week of pregnancy and in this time period both propylthiuracil and thiamazole (or methimazole) can be used.1
Our patient presented with an otherwise unexplained, persistent fetal tachycardia some years after radioactive iodine treatment for Grave’s disease. The fetus presented tricuspid insufficiency as a sign of beginning heart failure. The neonate was treated with b-blockers and thiamazole, the mother was allowed to breastfeed and the outcome was excellent.
Bibliography
- Alexander EK, Pearce EN, Brent GA et al (2017). 2017 guidelines of theAmerican Thyroid Association for the diagnosis and management of thyroid disease during pregnancy and the postpartum. Thyroid 27:315–389.
- Samuels, S. L., Namoc, S. M., & Bauer, A. J. (2018). Neonatal Thyrotoxicosis. Clinics in Perinatology, 45(1), 31–40. https://doi.org/https://doi.org/10.1016/j.clp.2017.10.001
- Iwen, K. A., & Lehnert, H. (2018). Schilddrüse und Schwangerschaft. Der Internist. https://doi.org/10.1007/s00108-018-0435-0
- Nguyen CT, Sasso EB, Barton L, Mestman JH. Graves’ hyperthyroidism in pregnancy: a clinical review. Clinical Diabetes and Endocrinology. 2018;4:4. doi:10.1186/s40842-018-0054-7.
- Berg, Cristoph. “12 Endokrine Erkrankungen und Stoffwechselstörungen.” Fetale Therapie, De Gruyter, 2017, pp. 263–268.
- Doucette S, Tierney A, Roggensack A, and Yusuf K. Neonatal Thyrotoxicosis with Tricuspid Valve Regurgitation and Hydrops in a Preterm Infant Born to a Mother with Graves’ Disease. AJP Rep. 2018 Apr; 8(2): e85-88. Published online 2018 May 4. doi: 10.1055/s-0038-1645879.
- Steiner H., Schneider K-T. M., Dopplersonographie in Geburtshilfe und Gynakologie. 3. Auflage. Berlin Heidelberg: Springer Verlag; c2012. Kapitel 21, Evaluierung des Cardiac Output und der kardialen Dekompensation; p. 230-235.
- Helfer, T., Peixoto, A., Tonni, G., & Araujo Júnior, E. (2016). Craniosynostosis: prenatal diagnosis by 2D/3D ultrasound, magnetic resonance imaging and computed tomography. Medical Ultrasonography, 18(3), 378-385. doi:http://dx.doi.org/10.11152/mu.2013.2066.183.3du
- Bernardes, L. S., Ruano, R. , Sapienza, A. D., Maganha, C. A. and Zugaib, M. (2008). Nomograms of fetal thyroid measurements estimated by 2‐dimensional sonography. J. Clin. Ultrasound, 36: 193-199. doi:10.1002/jcu.20434
- Ranzini, A. C., Ananth, C. V, Smulian, J. C., Kung, M., Limbachia, A., & Vintzileos, A. M. (2001). Ultrasonography of the fetal thyroid: nomograms based on biparietal diameter and gestational age. Journal of Ultrasound in Medicine, 20(6), 613–617. https://doi.org/10.7863/jum.2001.20.6.613
- Sato, Y., Murata, M., Sasahara, J., Hayashi, S., Ishii, K., & Mitsuda, N. (2014). A case of fetal hyperthyroidism treated with maternal administration of methimazole. Journal Of Perinatology, 34, 945. Retrieved from http://dx.doi.org/10.1038/jp.2014.163
A similar version of the above article was available as a poster during the 18th congress of the German society of prenatal and obstetric medicine, 8-9 June 2018 (DGPGM – Deutsche Gesellschaft für Pränatal- und Geburtsmedizin) and is available as an abstract here: https://www.thieme-connect.com/products/ejournals/abstract/10.1055/s-0038-1660618.