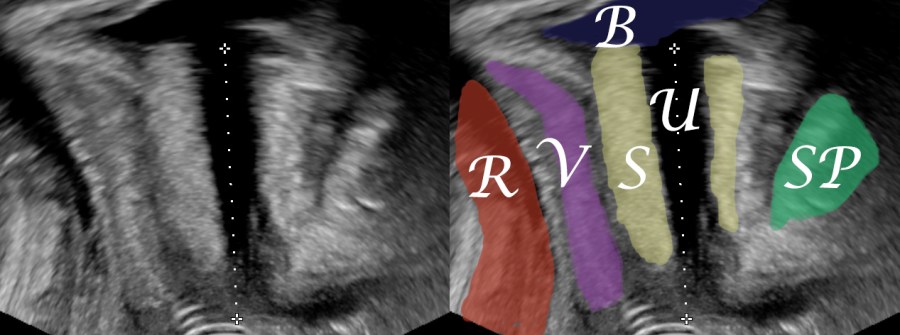
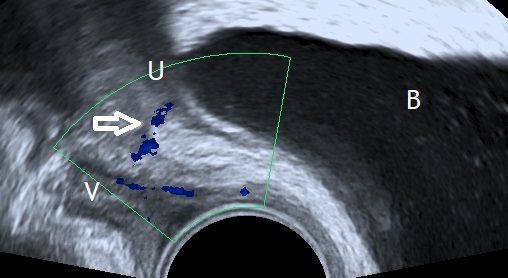
Definition
Levator avulsion is the traumatic disconnection of the puborectalis component
of the levator ani from the os pubis (Dietz, 2019).
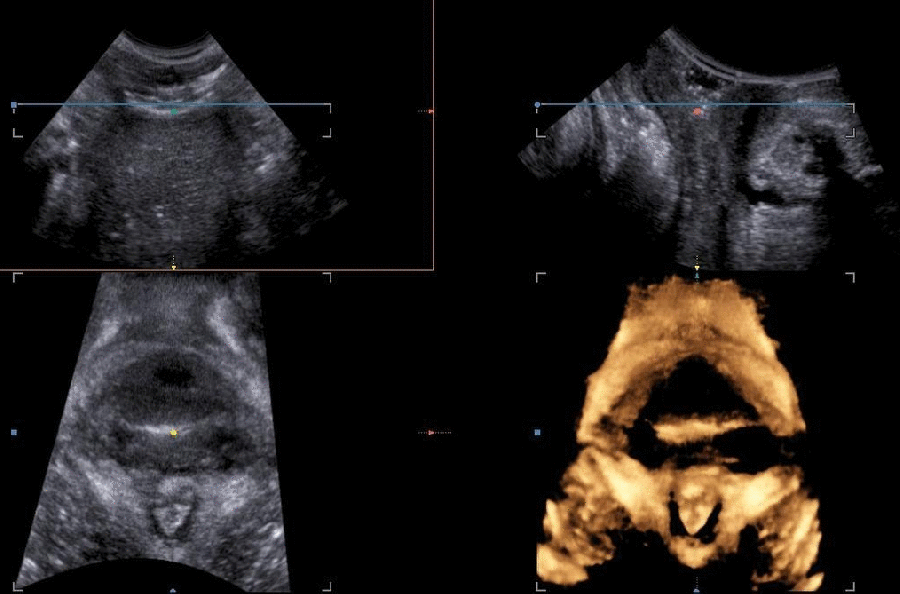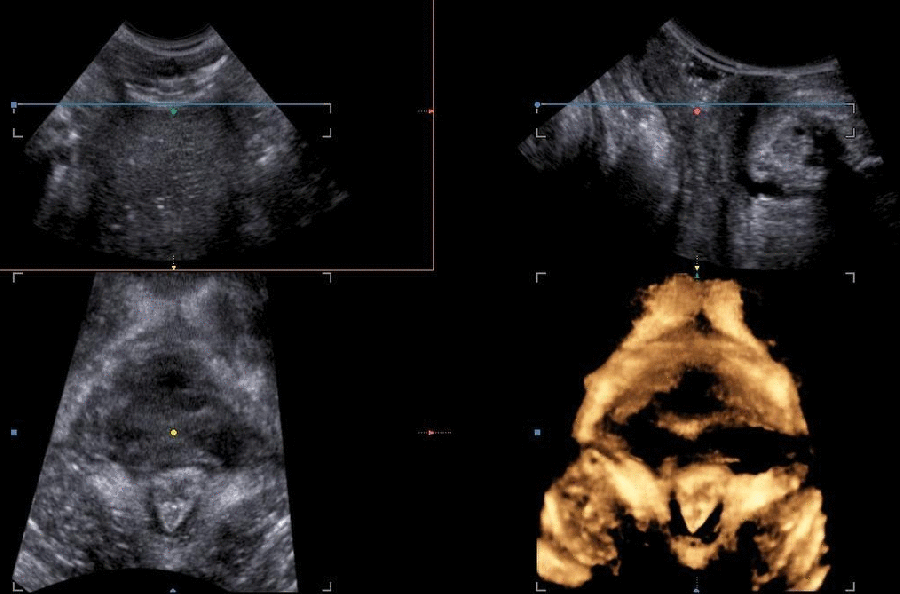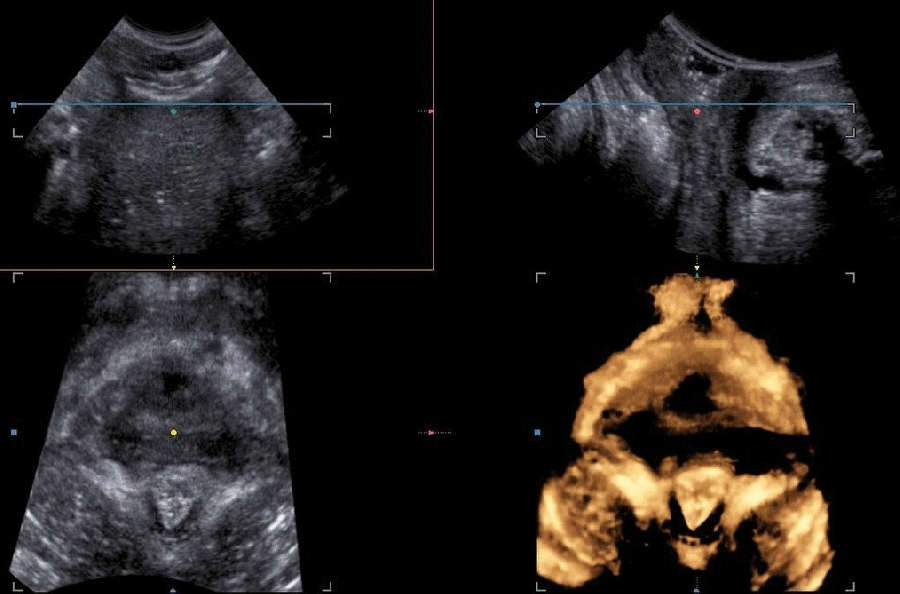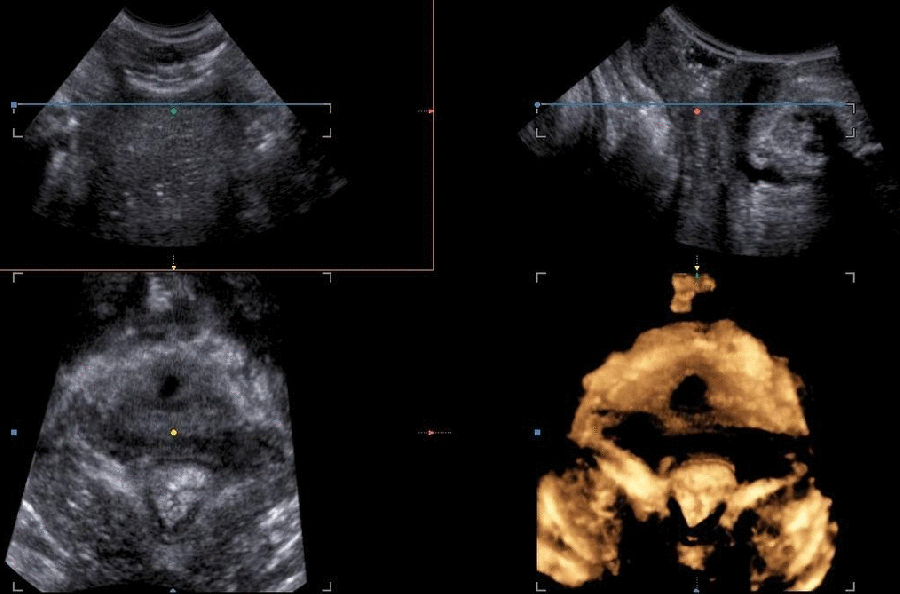
Types
The levator ani avulsion may be categorized as:
- LAM I, when there is obvious damage but the arch of the levator remains intact, and as
- LAM II, when there is complete detachment of the pubovisceral muscle from its insertion at the pubic level (García-Mejido, J. A., & Sainz, J. A., 2020).
Epidemiology/
Levator ani avulsion during vaginal delivery in primiparous women occurs in nearly 1/5 deliveries.
Risk Factors
- Primiparity
- Delivery mode (forceps bears the highest risk, vacuum delivery increases the risk only slightly)
- Length of second stage of delivery
- Neonatal birth weight
- Fetal head circumference
- OASIS (Obstetric Anal Sphincter Injuries)
- P-PPVD (Persistent Post-Partum Voiding Disorder)
- Kristeller-Maneuver
(Cassadó J. et al., 2020, Dietz 2019, Youssef, A. et al., 2019, Gonzalez-Díaz, E., & Biurrun, G. P., 2020, Kimmich, 2020).
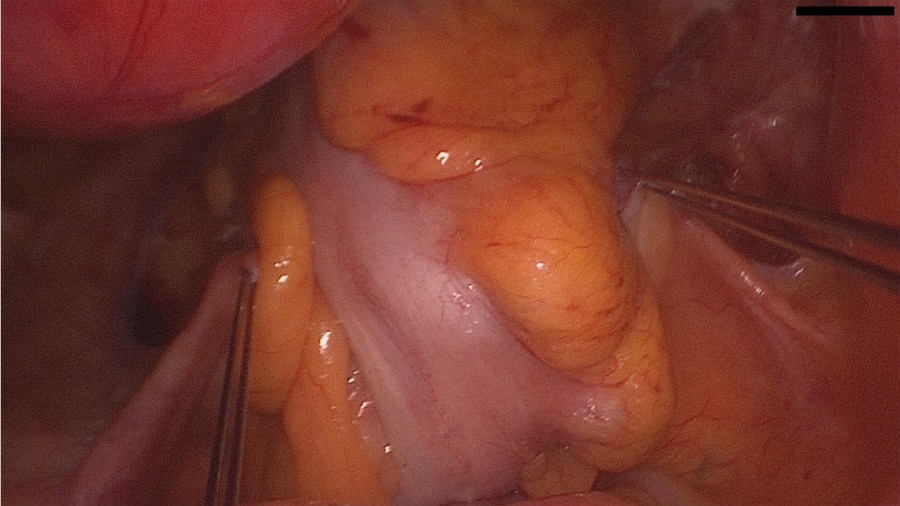
Clinical Image
Levator ani avulsion seems to have a causative effect on:
- Pelvic organ prolapse (especially cystocele and uterine descent)
- Poor muscle strength
- Sexual dysfunction
- Pelvic organ prolapse after surgery
(Handa et al, 2019, Handa et al, 2020, García-Mejido, J. A., et al., 2020, Dietz, 2019).
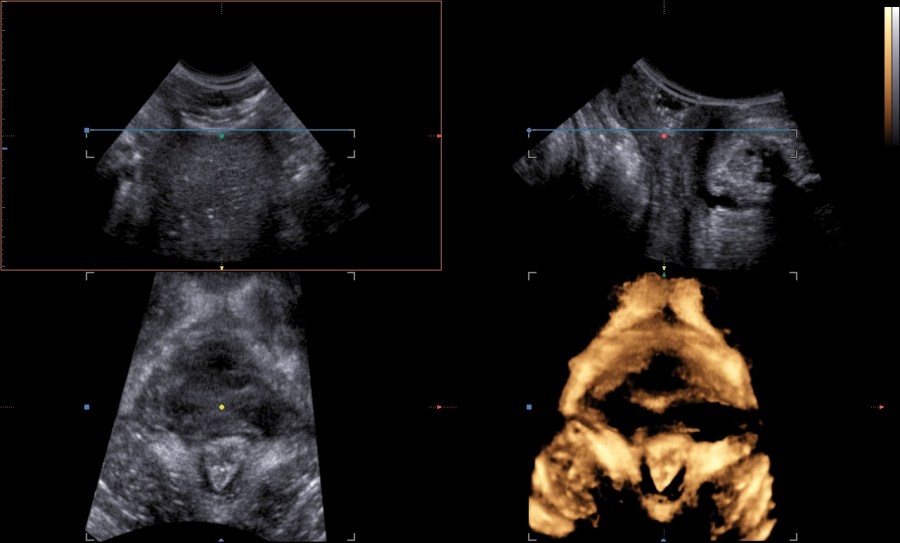
Histology
One recent study on cadavers tried to compare the sonographic levator ani muscle avulsion to findings from histology. The authors decided that the sonographic appearance of avulsion may not necessarily mean true separation of muscle from bone, but at least it definitely corresponds to muscle injury. Thus they suggested using the term “levator ani injury” should be more correct than the term “avulsion” (Da Silva et al, 2019).
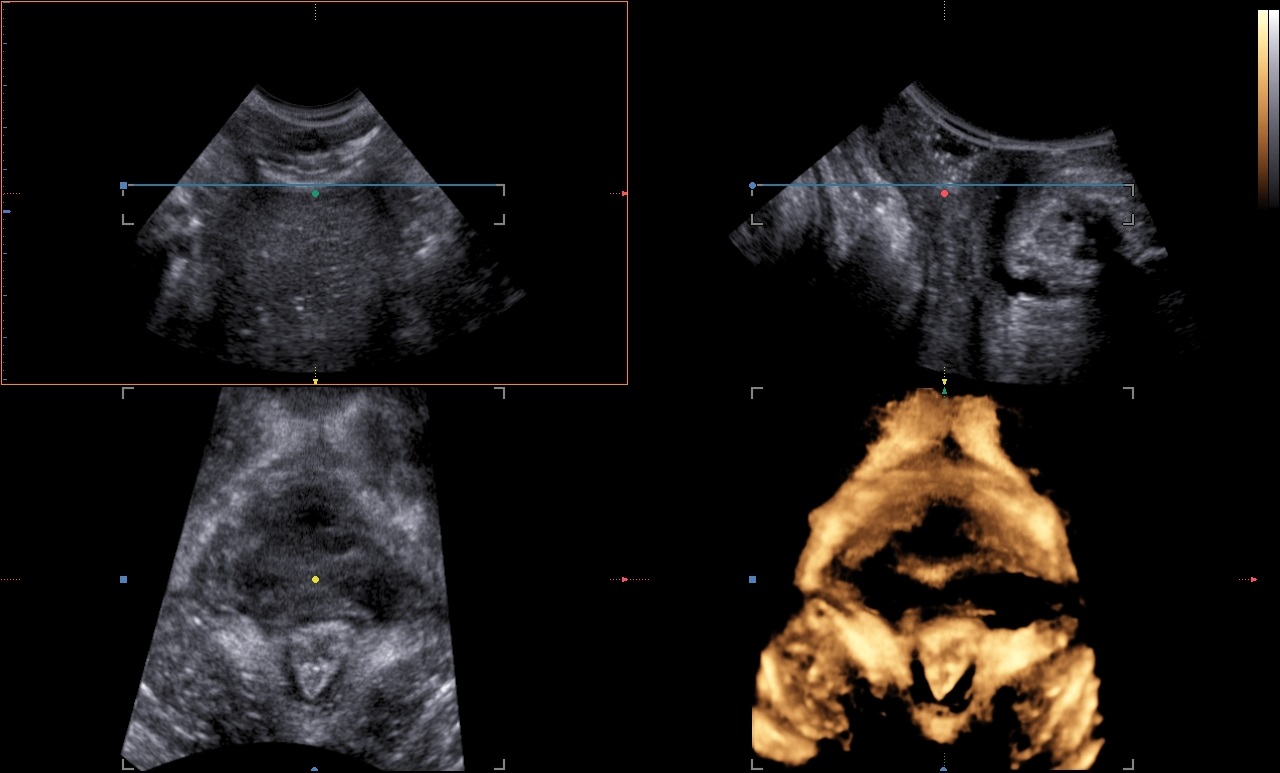
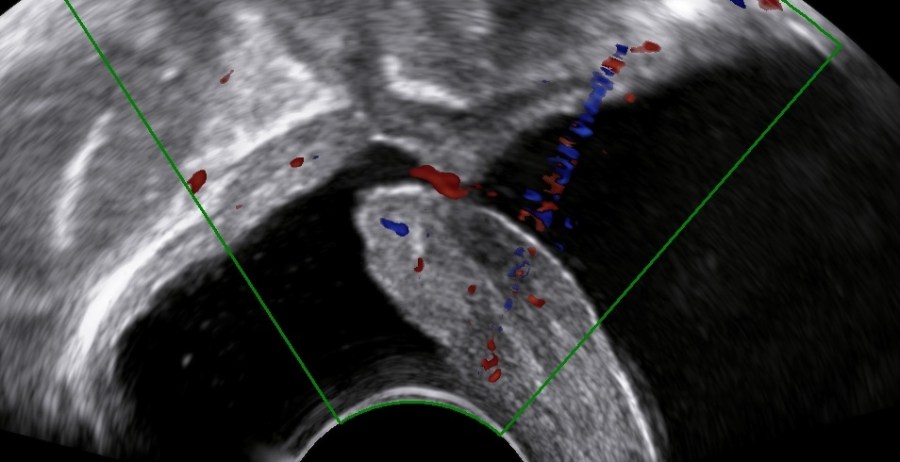
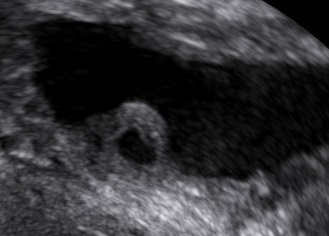
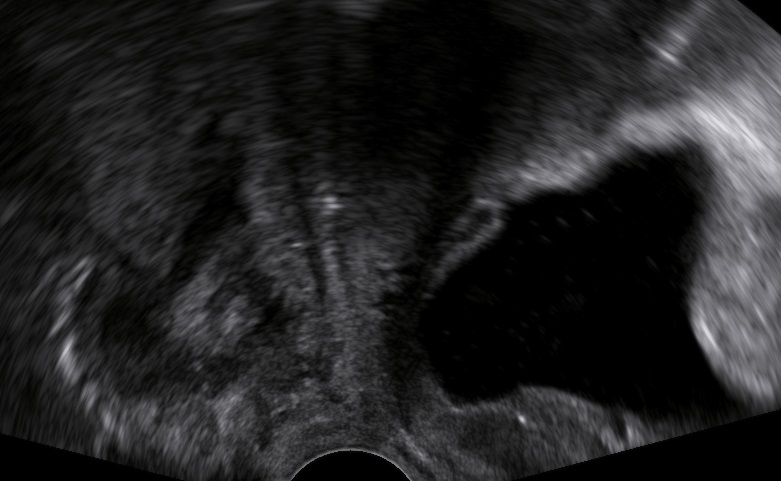
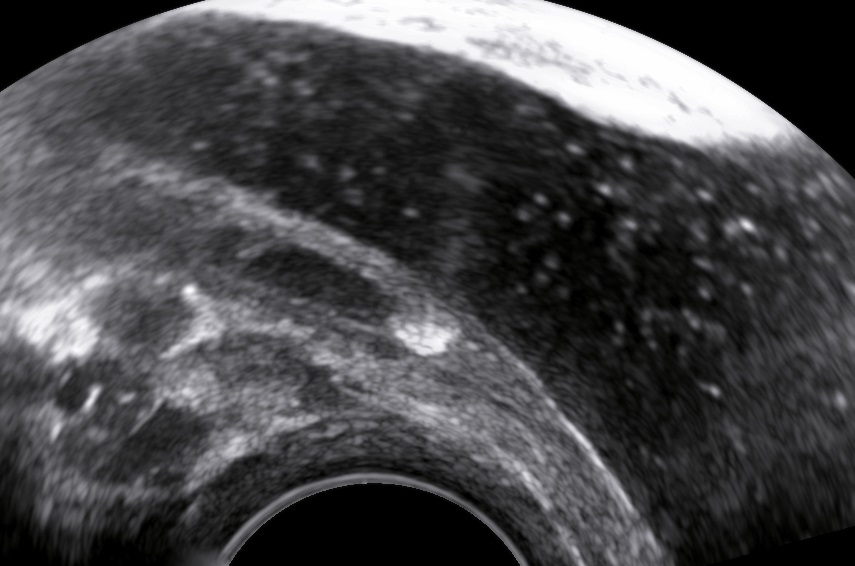
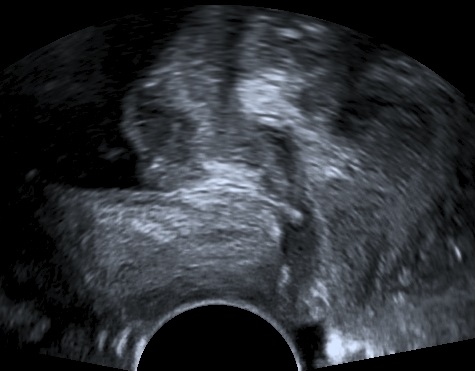
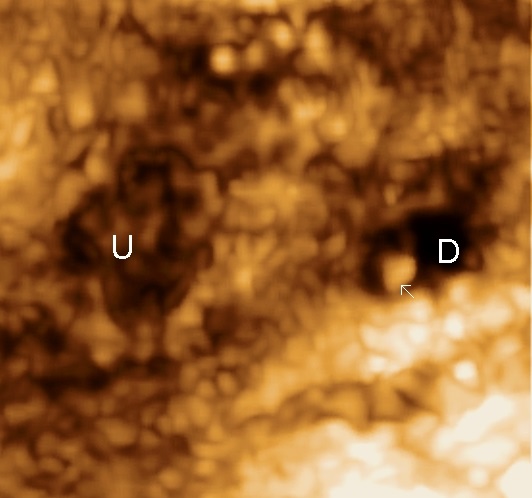
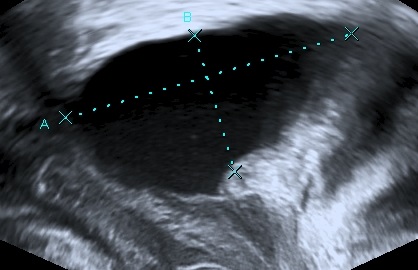
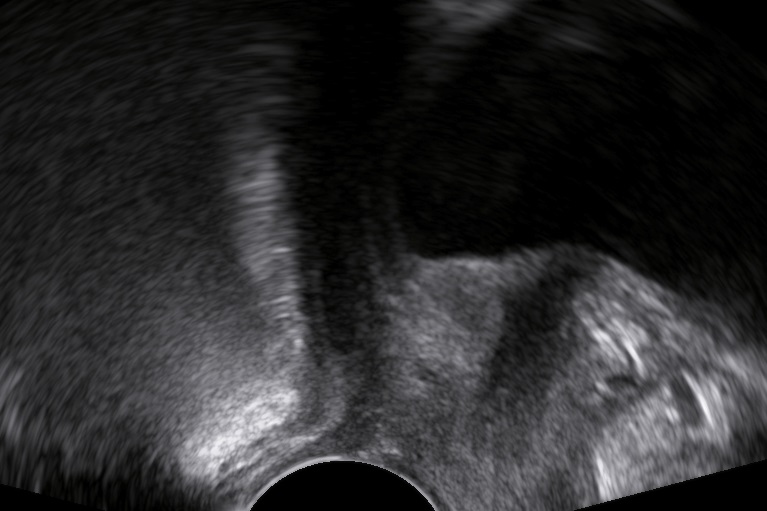
Diagnostics
The levator ani muscle avulsion may be demonstrated with 2D Ultrasound, however 3D (or even 4D) Ultrasound as well as MRI are superior in demonstrating avulsion (Dietz 2019).
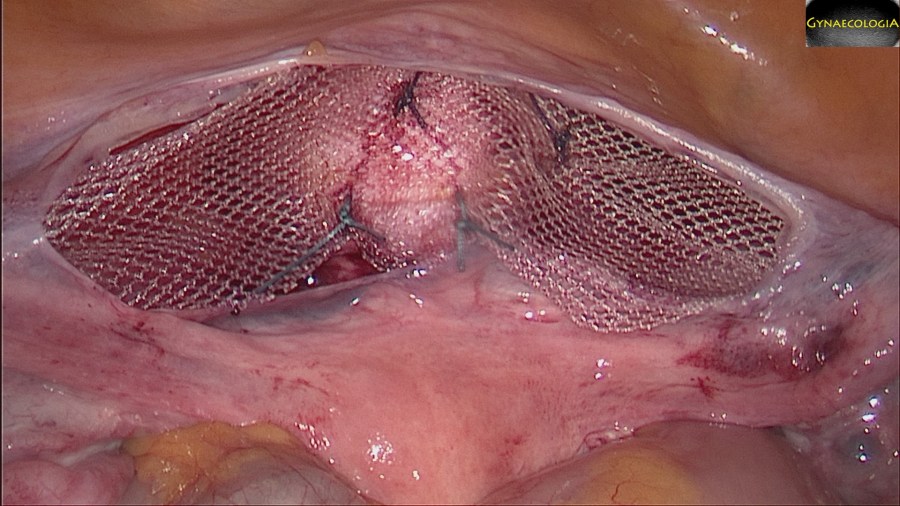
Management
In the presence of risk factors after a vaginal delivery we suggest:
- The early sonographic examination to detect a levator ani muscle avulsion
- Proper patient councelling about the future risks of an avulsion
- Consequential initiation of pelvic organ muscle training, even as prophylaxis at asymptomatic patients
In the primary investigation of pelvic organ prolapse we suggest:
- 3D sonography to detect a possible underlying levator ani muscle avulsion (Dietz, 2019)
- Proper patient preoperative councelling about the higher risk of recurrence after prolapse surgery
Prevention
Minimize the modifiable risk factors during delivery (van Delft K., et al., 2014):
- Reduce the rate of instrumental delivery and especially forceps
- Proper use of vacuum delivery (median sagittal placement at the flexion point)
- Better manual perineal protection
- Better fetal weight/fetal head circumference/maternal pelvis estimation and timely offering of cesarean section when cephalopelvic disproportion seems inevitable
- Minimize unnecesary Kristeller-Maneuver
- Reduce the length of the second stage of delivery through proper patient positioning, active guidance and use of oxytocin
Bibliography
- Handa, V. L., Roem, J., Blomquist, J. L., Dietz, H. P., & Muñoz, A. (2019). Pelvic organ prolapse as a function of levator ani avulsion, hiatus size, and strength. American journal of obstetrics and gynecology, 221(1), 41.e1–41.e7. https://doi.org/10.1016/j.ajog.2019.03.004
- Handa, V. L., Blomquist, J. L., Roem, J., Muñoz, A., & Dietz, H. P. (2020). Levator Morphology and Strength After Obstetric Avulsion of the Levator Ani Muscle. Female pelvic medicine & reconstructive surgery, 26(1), 56–60. https://doi.org/10.1097/SPV.0000000000000641
- Da Silva, A. S., Asfour, V., Digesu, G. A., Cartwright, R., Fernando, R., & Khullar, V. (2019). Levator Ani avulsion: The histological composition of this site. A cadaveric study. Neurourology and urodynamics, 38(1), 123–129. https://doi.org/10.1002/nau.23847
- Cassadó, J., Simó, M., Rodríguez, N., Porta, O., Huguet, E., Mora, I., Girvent, M., Fernández, R., & Gich, I. (2020). Prevalence of levator ani avulsion in a multicenter study (PAMELA study). Archives of gynecology and obstetrics, 302(1), 273–280. https://doi.org/10.1007/s00404-020-05585-4
- Youssef, A., Salsi, G., Cataneo, I., Pacella, G., Azzarone, C., Paganotto, M. C., Krsmanovic, J., Montaguti, E., Cariello, L., Bellussi, F., Rizzo, N., & Pilu, G. (2019). Fundal pressure in second stage of labor (Kristeller maneuver) is associated with increased risk of levator ani muscle avulsion. Ultrasound in obstetrics & gynecology : the official journal of the International Society of Ultrasound in Obstetrics and Gynecology, 53(1), 95–100. https://doi.org/10.1002/uog.19085
- Handa, V. L., Blomquist, J. L., Roem, J., Muñoz, A., & Dietz, H. P. (2019). Pelvic Floor Disorders After Obstetric Avulsion of the Levator Ani Muscle. Female pelvic medicine & reconstructive surgery, 25(1), 3–7. https://doi.org/10.1097/SPV.0000000000000644
- García-Mejido, J. A., & Sainz, J. A. (2020). Type of levator ani muscle avulsion as predictor for the disappearance of avulsion. Neurourology and urodynamics, 39(8), 2293–2300. https://doi.org/10.1002/nau.24484
- García-Mejido, J. A., Idoia-Valero, I., Aguilar-Gálvez, I. M., Borrero González, C., Fernández-Palacín, A., & Sainz, J. A. (2020). Association between sexual dysfunction and avulsion of the levator ani muscle after instrumental vaginal delivery. Acta obstetricia et gynecologica Scandinavica, 99(9), 1246–1252. https://doi.org/10.1111/aogs.13852
- van Gruting, M. A., van Delft, K., Sultan, A. H., & Thakar, R. (2020). The natural history of Levator ANI Muscle Avulsion 4 years following childbirth. Ultrasound in obstetrics & gynecology : the official journal of the International Society of Ultrasound in Obstetrics and Gynecology, 10.1002/uog.23120. Advance online publication. https://doi.org/10.1002/uog.23120
- Gonzalez-Díaz, E., & Biurrun, G. P. (2020). Levator ani muscle avulsion: a risk factor for persistent postpartum voiding dysfunction. International urogynecology journal, 31(11), 2327–2335. https://doi.org/10.1007/s00192-020-04412-3
- Dietz H. P. (2019). Ultrasound in the assessment of pelvic organ prolapse. Best practice & research. Clinical obstetrics & gynaecology, 54, 12–30. https://doi.org/10.1016/j.bpobgyn.2018.06.006
- Kimmich, N., Birri, J., Zimmermann, R., & Kreft, M. (2020). Prediction of levator ani muscle avulsion by genital tears after vaginal birth-a prospective observational cohort study. International urogynecology journal, 31(11), 2361–2366. https://doi.org/10.1007/s00192-020-04297-2
- van Delft, K., Thakar, R., Sultan, A. H., Schwertner-Tiepelmann, N., & Kluivers, K. (2014). Levator ani muscle avulsion during childbirth: a risk prediction model. BJOG : an international journal of obstetrics and gynaecology, 121(9), 1155–1163. https://doi.org/10.1111/1471-0528.12676