Gastroschisis comes from the greek words γᾰστήρ and σχίσις, which translate into abdomen and fissure respectively.1 It refers to an abdominal wall defect of varying size typically on the right side of the umbilicus and usually presents with small intestine prolapse into the amniotic fluid.2
Epidemiology and Risk Factors
Gastroschisis has an increasing incidence from 0.1/10.000 births in 1970 to 5/10.000 in 2000. Younger maternal age, smoking, a history of pregestational or gestational diabetes and use of antidepressants have been recognized as significant risk factors of gastroschisis.3
Genetics and Councelling
Genetic testing should be kept for cases of gastroschisis where associated anatomic malformations (15% of cases), suspicion of ruptured omphalocele, or positive first or second trimester serum screening coexist. The total percentage of infants with gastroschisis and abnormal karyotype is about 1%. An association with amyoplasia in about 0.5-3.2% of cases has also been described. The estimated sibling recurrence risk is 3.5%.1
Appearance
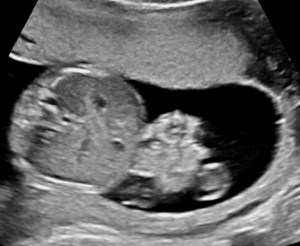
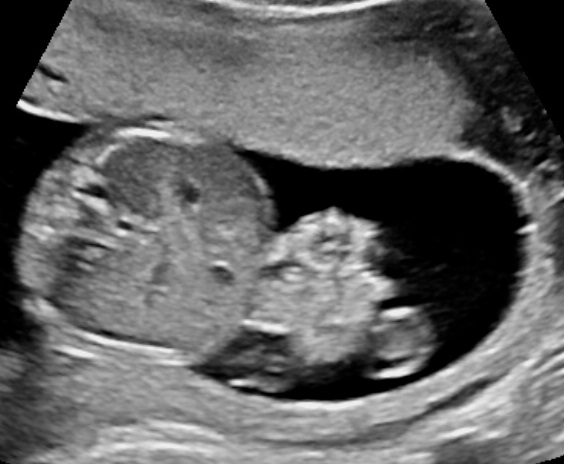
The characteristic ultrasound appearance of gastroschisis is that of cauliflower‐like intestinal loops floating in the amniotic fluid.4
Prognosis
Survival rate after surgery reaches more than 90%. Gastrointestinal complications in later life are not rare, mainly involving symptoms like constipation, chronic pain or reflux, while the risk of short bowel syndrome is also present. If the gonads are involved, future fertility may also be affected. The quality of life can be excellent.1
Complications
1. Intrauterine growth restriction (IUGR) in 30-50% of cases.1
2. Preterm labor in about 28% of cases.1
3. Bowel injury, whereas short bowel syndrome complicates 4.1% to 9.8% of gastroschisis cases.1 Bowel perforation is a very rare yet dangerous complication.6
4. Intrauterine fetal demise (IUFD) in about 4.5% of cases. The risk is increased with increasing gestational age particularly at 38 weeks and beyond.5
5. Obstruction of the urinary tract.7
6. Polyhydramnios, which is strongly predictive of severe bowel complications in the neonatal period.8
Late Onset Gastroschisis
Blondiaux et al. described a case of late onset gastroschisis which appeared only late during the third trimester while previous examinations (even with MRI) didn’t show any bowel loop herniation. This could explain how some cases of gastroschisis could be missed.4
Vanishing Gastroschisis
The spontaneous closure of an abdominal wall defect, which sometimes happens during the third trimester, is not a good prognostic sign and has been associated with prolonged initial hospitalization, multiple surgeries and higher incidence of short bowel syndrome.2
Ultrasound Surveillance Protocoll
We suggest always a thorough ultrasound scan in search for associated anomalies, which can be found in about 15% of the cases. Regular ultrasound examinations (e.g. biweekly up to 33 weeks, then once a week) with estimation of: fetal growth, amniotic fluid, doppler of the umbilical artery, fetal bowel appearance.9
Measurement of the bowel lumen should be performed with calipers on to on from inner wall to inner wall at a right angle with the bowel wall at the point of maximum dilatation. Sustained, increasing dilatation of the intra-abdominal bowel (at least > 6 mm) especially in the third trimester has been associated with fetuses that develop bowel obstruction requiring surgery after birth.9,10,11
Timing of Delivery
Delivering the fetus with gastroschisis at early term (37–38 weeks) has been associated with decreased risk of stillbirth and death within 1 year of delivery.12 The fetal gastroschisis is not a contraindication for vaginal delivery. Delivery should be performed at a specialized unit.13
Bibliography
- Lepigeon, K. , Van Mieghem, T. , Vasseur Maurer, S. , Giannoni, E. and Baud, D. (2014), Gastroschisis – what should be told to parents?. Prenat Diagn, 34: 316-326. doi:10.1002/pd.4305
- Ponce, M. M., Hermans, D., de Magnee, C., Hubinont, C., & Biard, J.-M. (2018). Vanishing gastroschisis visualized by antenatal ultrasound: a case report and review of literature. European Journal of Obstetrics and Gynecology and Reproductive Biology, 228, 186–190. https://doi.org/10.1016/j.ejogrb.2018.06.028
- Skarsgard, E. D., Meaney, C. , Bassil, K. , Brindle, M. , Arbour, L. , Moineddin, R. (2015), Maternal risk factors for gastroschisis in Canada. Birth Defects Research Part A: Clinical and Molecular Teratology, 103: 111-118. doi:10.1002/bdra.23349
- Blondiaux, E. , Guilbaud, L. , Auber, F. , Rosenblatt, J. , Richard, F. , Jouannic, J. , Pointe, H. D. and Garel, C. (2012), A challenging case of late‐onset gastroschisis. Ultrasound Obstet Gynecol, 40: 610-611. doi:10.1002/uog.11153
- Meyer, M. R., Shaffer, B. L., Doss, A. E., Cahill, A. G., Snowden, J. M., & Caughey, A. B. (2014). Prospective risk of fetal death with gastroschisis. The Journal of Maternal-Fetal & Neonatal Medicine, 28(17), 2126–2129. doi:10.3109/14767058.2014.984604
- Haberman, S. , Burgess, T. , Klass, L. , Cohn, B. D. and Minkoff, H. L. (2000), Acute bowel perforation in a fetus with gastroschisis. Ultrasound Obstet Gynecol, 15: 542-544. doi:10.1046/j.1469-0705.2000.00039.x
- Reiss, R. , Landon, M. , Jayanthi, V. , Caniano, D. , Mutabagani, K. and O’Shaughnessy, R. (2000), Functional urinary tract obstruction developing in fetuses with isolated gastroschisis. Ultrasound in Obstetrics and Gynecology, 15: 194-198. doi:10.1046/j.1469-0705.2000.00003.x
- Peter, J. R., Chan, F. Y. and Hockey, R. (2001), Gastroschisis – can prenatal ultrasonography predict neonatal outcome?. Ultrasound in Obstetrics and Gynecology, 18: F68-F68. doi:10.1046/j.1469-0705.2001.0180S1029.x
- Brantberg, A. , Blaas, H. K., Salvesen, K. Å., Haugen, S. E. and Eik‐nes, S. H. (2004), Surveillance and outcome of fetuses with gastroschisis. Ultrasound Obstet Gynecol, 23: 4-13. doi:10.1002/uog.950
- Contro, E. , Fratelli, N. , Okoye, B. , Papageorghiou, A. , Thilaganathan, B. and Bhide, A. (2010), Prenatal ultrasound in the prediction of bowel obstruction in infants with gastroschisis. Ultrasound Obstet Gynecol, 35: 702-707. doi:10.1002/uog.7514
- Nick, A. M., Bruner, J. P., Moses, R. , Yang, E. Y. and Scott, T. A. (2006), Second‐trimester intra‐abdominal bowel dilation in fetuses with gastroschisis predicts neonatal bowel atresia. Ultrasound Obstet Gynecol, 28: 821-825. doi:10.1002/uog.2858
- Harper, L. M., Goetzinger, K. R., Biggio, J. R. and Macones, G. A. (2015), Timing of elective delivery in gastroschisis: a decision and cost‐effectiveness analysis. Ultrasound Obstet Gynecol, 46: 227-232. doi:10.1002/uog.14721
- Friedman, A. M., Ananth, C. V., Siddiq, Z., D’Alton, M. E., & Wright, J. D. (2016). Gastroschisis: epidemiology and mode of delivery, 2005-2013. American journal of obstetrics and gynecology, 215(3), 348.e1-9.
https://baileypetrucelli.wordpress.com/2018/12/27/gastroschisis-baby-how-to-stay-positive-when-your-birth-plans-dont-go-accordingly/
Praying for all mamas and babies out there! I am a mama who has a baby on the way with gastroschisis. I wrote a little bit about my experience so far and how to stay positive. Hope this can help anyone out there who is struggling or going through the same thing!
LikeLike