The pathogenesis of diabetic cardiomyopathy is multifactorial and is not fully understood (Stuart et al, 2010). It is observed in infants of diabetic mothers whether or not there is reasonable metabolic control (Hornberger, 2006). Up to 50% of newborn infants of Type 1 diabetic mothers can be diagnosed with hypertrophic cardiomyopathy (Kulkarni et al, 2017).
Diagnosing hypertrophic cardiomyopathy
Thickening of the interventricular septum, and to a lesser extent the ventricular free walls (Hornberger, 2006). This thickening can lead to ventricular outflow obstruction (Stuart et al, 2010). The thickness of the interventricular septum should be measured at the four chamber view, just below the level of the atrioventricular valves in end diastole (Kulkarni et al, 2017).
Measurement of the diastolic function, or E/A ratio could also be useful, because maternal diabetes has been shown to lead to a deterioration in fetal cardiac diastolic function especially of the right ventricle (Dervisoglu et al, 2018).
On a pulsed doppler examination just below the mitral valve and while keeping the gate size between 1-3 mm one could calculate the myocardial performance index (MPI). The formula devised from Tei et al is: (Isovolumic relaxation time + isovolumic contraction time) / ejection time. To make matters simpler, the MPI can also be calculated as (Mitral valve closure to opening time – ejection time) / ejection time (Tei et al, 1995).
The pulsatility index of the ductus venosus may be increased in fetuses of pregnancies complicated by pre‐existing diabetes mellitus as well as in pregnancies complicated by gestational diabetes, compared to fetuses of non-diabetic mothers (Stuart et al, 2010).
Two‐dimensional speckle‐tracking echocardiography is also very useful in diagnosing functional anomalies, like hypertrophic cardiomyopathy (Kulkarni et al, 2017).
Prognosis
Most affected infants are clinically asymptomatic and have resolution of the hypertrophy within months (Hornberger, 2006).
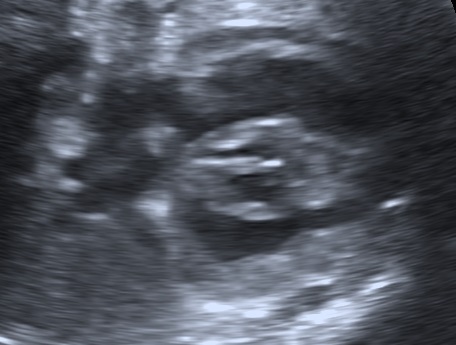
Below a case of fetal hypertrophic cardiomyopathy by maternal gestational diabetes mellitus in the 35w4d.
Bibliography
- Hornberger, L. K. (2006). Maternal diabetes and the fetal heart. Heart, 92(8), 1019–1021. http://doi.org/10.1136/hrt.2005.083840
- Stuart, A. , Amer‐Wåhlin, I. , Gudmundsson, S. , Maršál, K. , Thuring, A. and Källen, K. (2010), Ductus venosus blood flow velocity waveform in diabetic pregnancies. Ultrasound Obstet Gynecol, 36: 344-349. doi:10.1002/uog.7573
- Tei C, Ling LH, Hodge DO, et al. New index of combined systolic and diastolic myocardial performance: a simple and reproducible measure of cardiac function – a study in normals and dilated cardiomyopathy. J Cardiol 1995;26:357-366.
- Kulkarni, A. , Li, L. , Craft, M. , Nanda, M. , Lorenzo, J. M., Danford, D. and Kutty, S. (2017), Fetal myocardial deformation in maternal diabetes mellitus and obesity. Ultrasound Obstet Gynecol, 49: 630-636. doi:10.1002/uog.15971
- Dervisoglu, P., Kosecik, M., & Kumbasar, S. (2018). Effects of gestational and pregestational diabetes mellitus on the foetal heart: a cross-sectional study. Journal of Obstetrics and Gynaecology, 38(3), 408–412. doi:10.1080/01443615.2017.1410536