Definition
The mucinous cystadenoma is a benign mucinous ovarian neoplasm.

Epidemiology
Mucinous neoplasms of the ovary account for about 10%–15% of all ovarian neoplasms. They are divided as follows:
- Benign mucinous neoplasms (80%, patient age usually from 20s to 40s)
- mucinous cystadenoma and
- mucinous adenofibroma
- Borderline tumors (17%, patient age usually from 40-49 years)
- mucinous borderline tumor
- atypical proliferative mucinous tumor
- Mucinous carcinomas (3%, patient age usually about 45 years) (Marko J., et al, 2019).
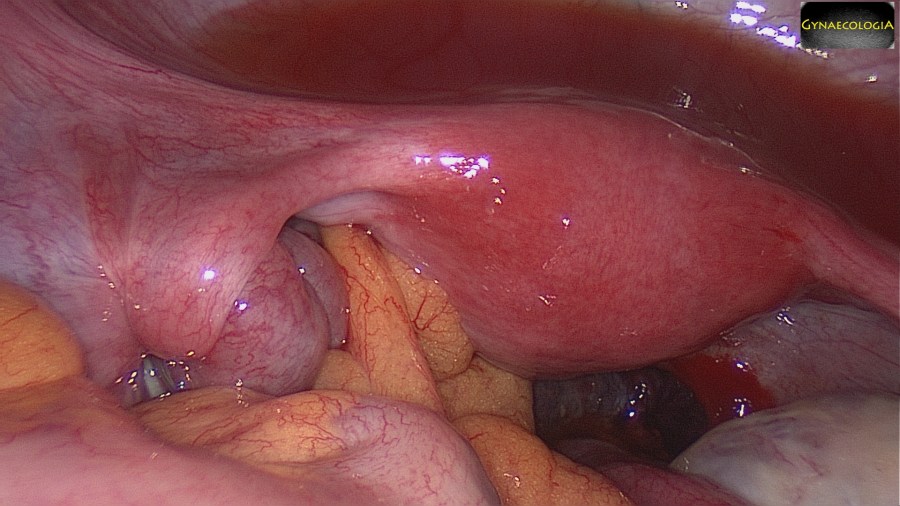
Clinical Image
- Lower abdominal pain.
- Abdominal fullness.
- Palpable mass.
- Distention of the abdomen (Marko J., et al, 2019).
Diagnostics
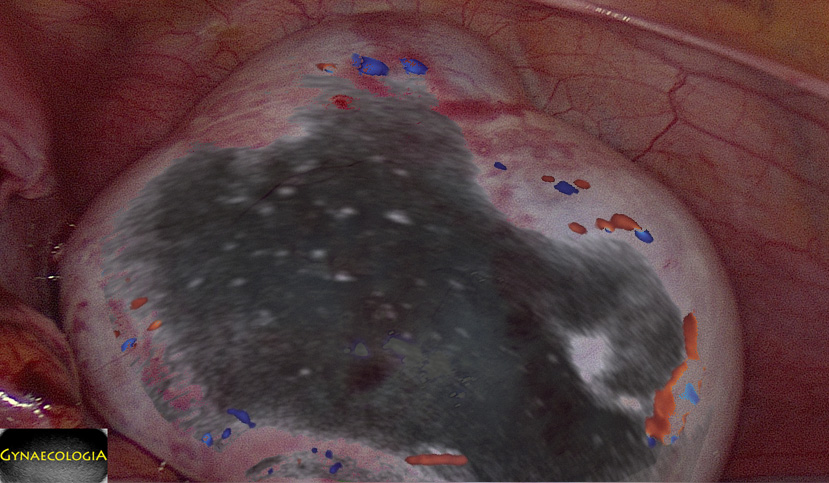
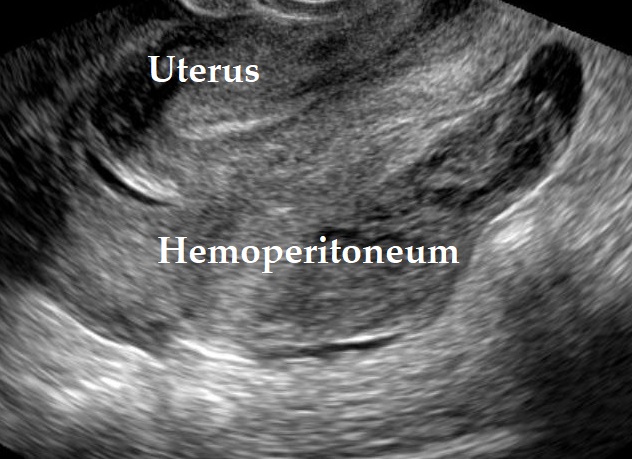
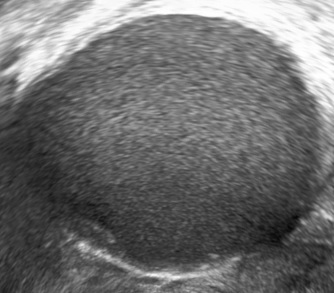
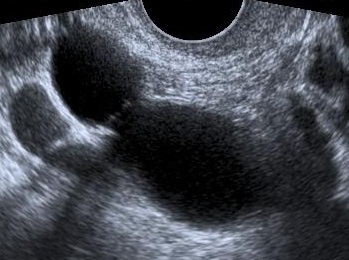
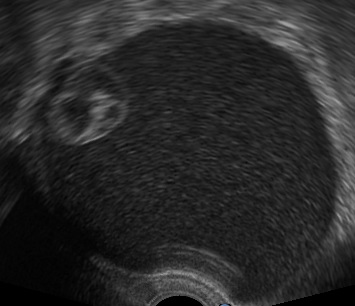
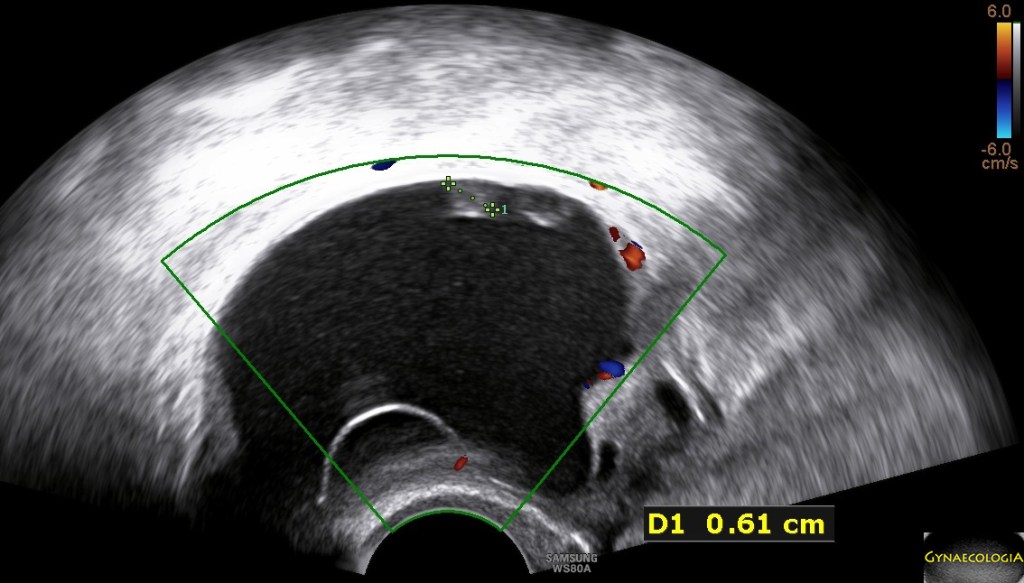
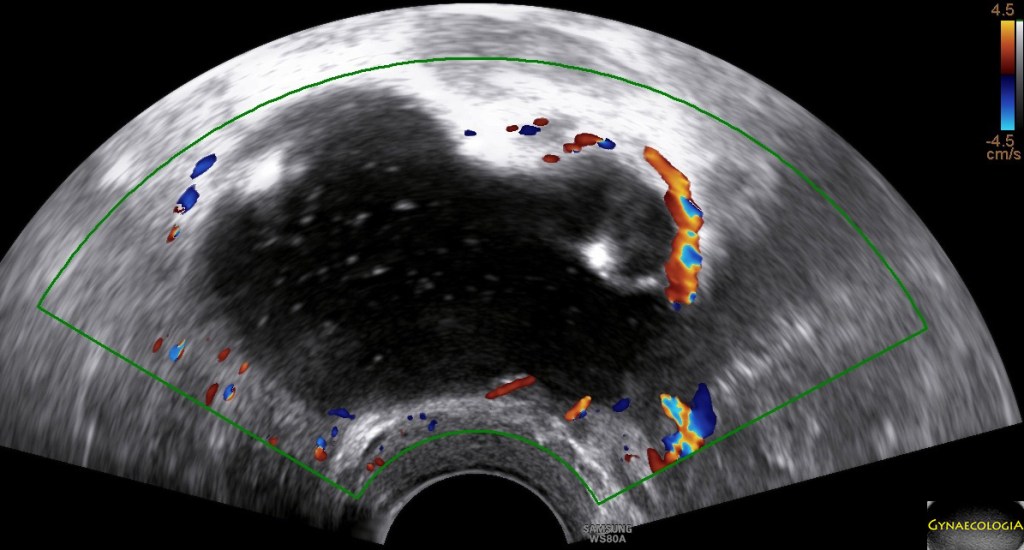
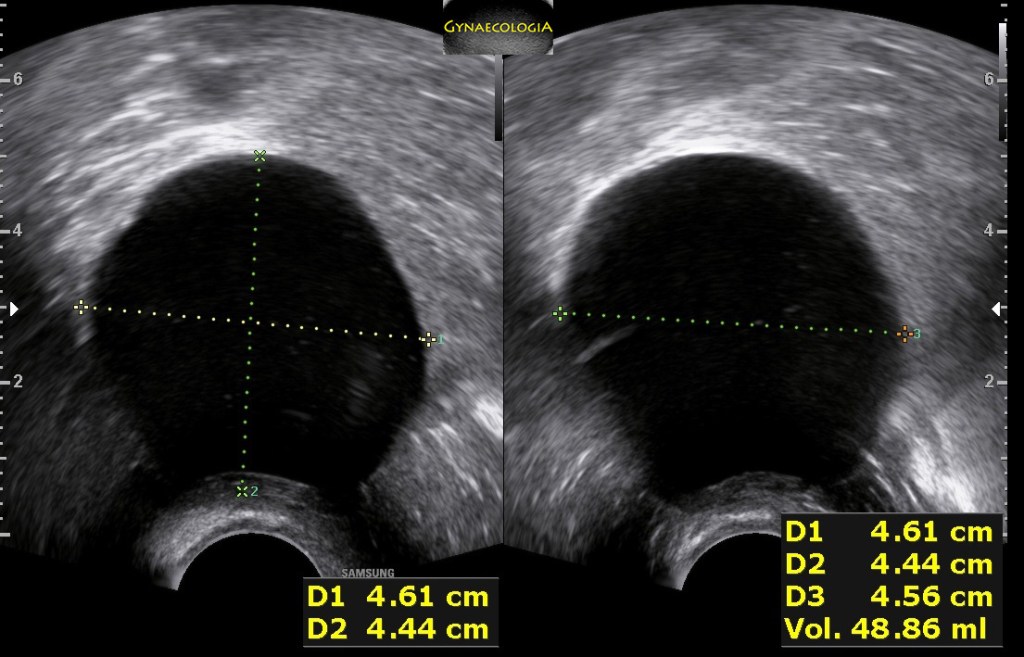
Ultrasound findings
- Frequently large, unilateral, cystic mass.
- Usually multilocular.
- Smooth walls.
- Contains small cystic components or honeycomb-like loculi.
- Intralocular fluid of varying echogenicity.
- Linear calcifications (rare).
- Papillary projections (rare).
- Mucinous ascites may present after cyst rupture.
From a pathology point-of-view, don’t forget that concomitant findings may include Brenner tumors, teratomas, and sarcoma-like mural nodules adding their respective ultrasound findings. (Mills A.M. & Shanes E.D., 2019).
Differential Diagnosis
Mucinous carcinoma – The following are characteristics of ovarian tumors that may imply malignancy:
- Thick irregular wall
- Thick septa
- Papillary projections
- Large soft-tissue component with necrosis
- Ancillary findings of pelvic organ invasion, spread to the peritoneum, omentum, or mesentery; ascites; and adenopathy are also suggestive of malignancy (Marko J., et al, 2019).
Pseudomyxoma peritonei – Typically has all of the following characteristics:
- Mucinous ascites
- Peritoneal implants
- Mucinous tumor of the appendix
Only rarely does a pseudomyxoma peritonei develop from a primary ovarian neoplasia (mature teratoma containing a mucinous neoplasm) (Carr, N. J., et al., 2016).
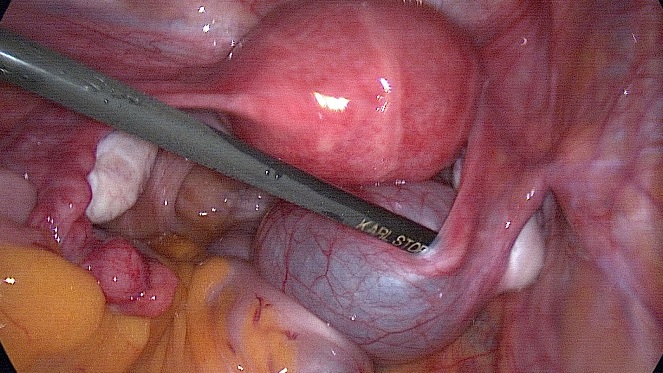
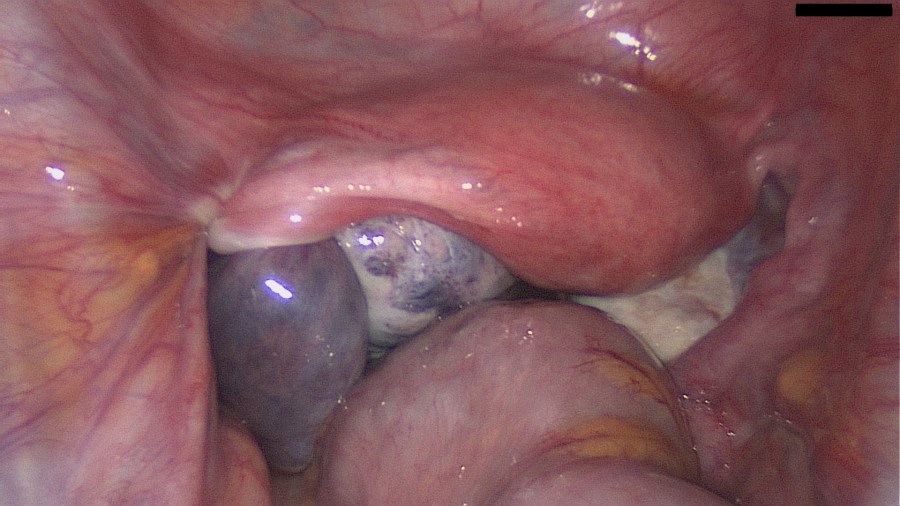
Management
Treatment of a mucinous cystadenoma is surgical.
Removal of the cyst alone has a high risk of recurrence.
Spillage of the contents of the cyst should be avoided.
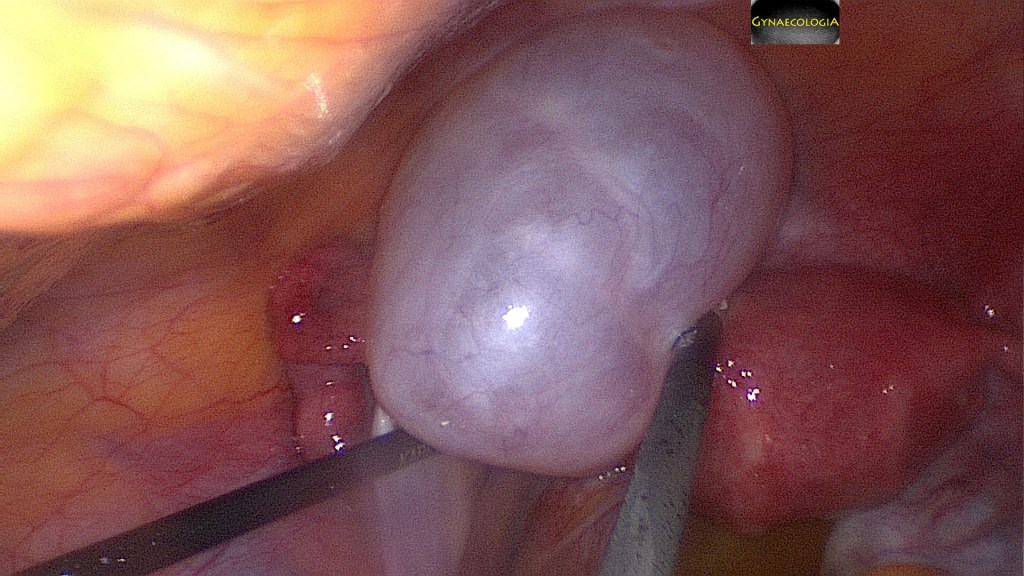
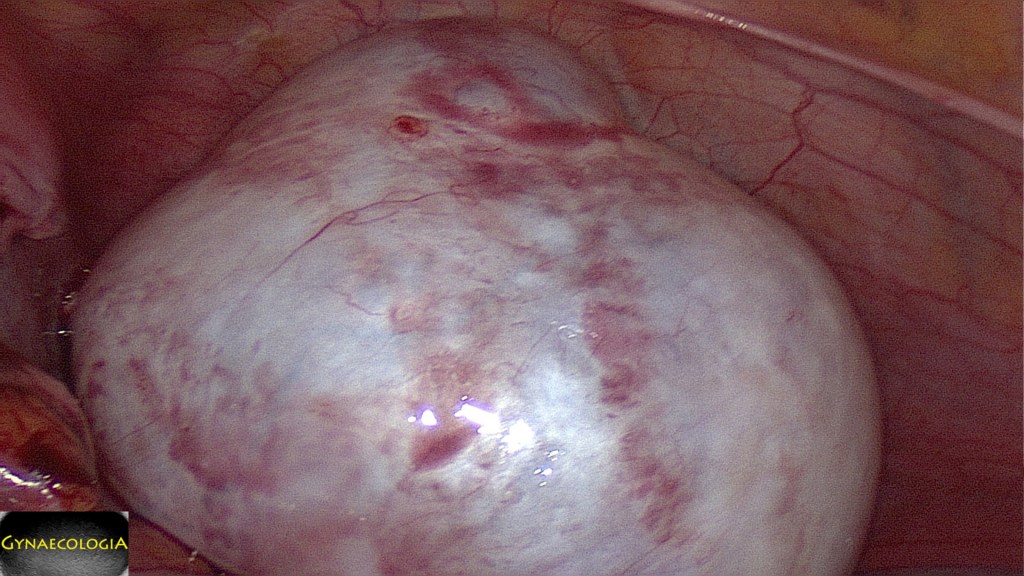
The intact removal of the ovary is suggested. This may be achieved either by laparotomy or laparoscopy. In the absence of malignancy and/or pseudomyxoma peritonei the mere inspection of the normal appendix suffices (Brown, J., & Frumovitz, M., 2014).
Bibliography
- Mills, A. M., & Shanes, E. D. (2019). Mucinous Ovarian Tumors. Surgical pathology clinics, 12(2), 565–585. https://doi.org/10.1016/j.path.2019.01.008
- Marko, J., Marko, K. I., Pachigolla, S. L., Crothers, B. A., Mattu, R., & Wolfman, D. J. (2019). Mucinous Neoplasms of the Ovary: Radiologic-Pathologic Correlation. Radiographics : a review publication of the Radiological Society of North America, Inc, 39(4), 982–997. https://doi.org/10.1148/rg.2019180221
- Carr, N. J., Cecil, T. D., Mohamed, F., Sobin, L. H., Sugarbaker, P. H., González-Moreno, S., Taflampas, P., Chapman, S., Moran, B. J., & Peritoneal Surface Oncology Group International (2016). A Consensus for Classification and Pathologic Reporting of Pseudomyxoma Peritonei and Associated Appendiceal Neoplasia: The Results of the Peritoneal Surface Oncology Group International (PSOGI) Modified Delphi Process. The American journal of surgical pathology, 40(1), 14–26. https://doi.org/10.1097/PAS.0000000000000535
- Brown, J., & Frumovitz, M. (2014). Mucinous tumors of the ovary: current thoughts on diagnosis and management. Current oncology reports, 16(6), 389. https://doi.org/10.1007/s11912-014-0389-x
Before you go, you might like other published articles on benign adnexal pathology:
And don’t forget to subscribe to stay always up to date: